Ambriel vs Assured
Side-by-side comparison to help you choose the right tool.
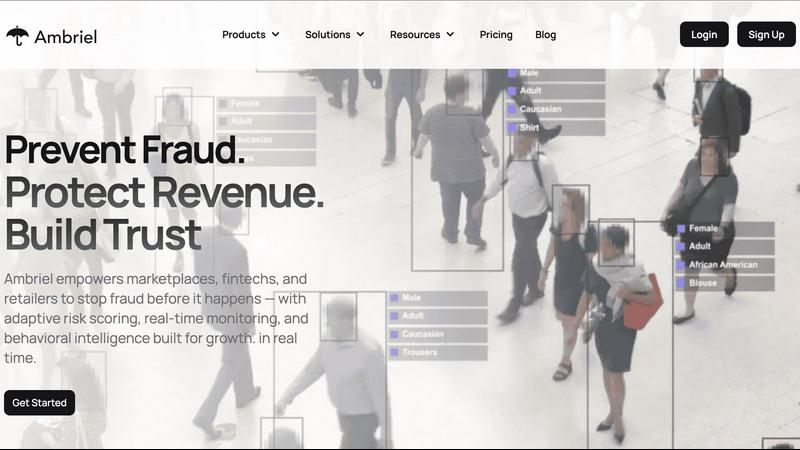
Ambriel prevents fraud in real time, safeguarding your revenue and ensuring trust across all transactions effortlessly.
Last updated: March 1, 2026
Assured
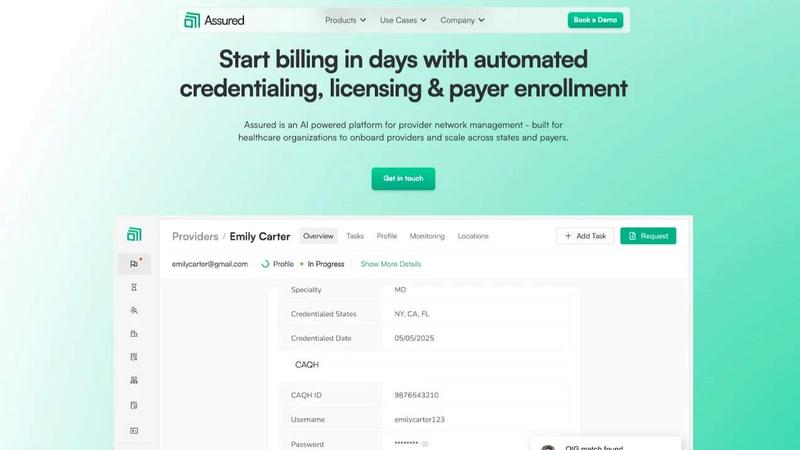
Assured automates provider credentialing and enrollment, enabling healthcare organizations to start billing in days instead of months.
Last updated: April 13, 2026
Visual Comparison
Ambriel
Assured
Feature Comparison
Ambriel
Advanced Fraud Detection
Ambriel leverages AI-driven risk scoring from over 200 data sources to identify suspicious activity in real-time. This feature is essential for protecting revenue, allowing businesses to act swiftly before fraudulent transactions impact their bottom line.
Sanctions & PEP Screening
This feature automates the screening process against over 100 global sanctions, politically exposed persons (PEP), and crime lists, eliminating the need for manual checks. It ensures that businesses remain compliant with regulations while maintaining operational efficiency.
Continuous Monitoring
Ambriel provides 24/7 tracking of transactions and accounts, alerting businesses to unusual patterns before they escalate into costly fraud cases. This continuous oversight is vital for maintaining a secure operational environment.
Seamless Onboarding
With customizable onboarding flows that include automated checks, Ambriel enables businesses to onboard only trusted customers and sellers. This reduces the risk of fraudulent accounts gaining access to the platform, enhancing overall security.
Assured
Automated Credentialing
Assured revolutionizes the credentialing process by automating primary source verifications and document management, reducing the onboarding time to mere days. This feature ensures that healthcare providers can be credentialed swiftly and accurately without the manual labor that typically slows down operations.
Multi-State Licensing
The platform simplifies the often chaotic process of multi-state licensing and renewals. Assured automatically tracks licensure expirations, submits applications, and manages renewals across all 50 states, eliminating the administrative burden and allowing healthcare organizations to scale seamlessly.
Streamlined Payer Enrollment
Assured accelerates the payer enrollment process, helping organizations get in-network 30% faster. This feature automates submissions and provides real-time tracking for enrollments and follow-ups, ensuring that no deadlines are missed and that providers can start seeing patients sooner.
Centralized Network Management
With Assured's centralized roster management, all provider data is consolidated in one location, allowing for real-time monitoring and verification from over 2,000 primary sources. This feature mitigates surprises during audits and enhances data integrity across the board.
Use Cases
Ambriel
Onboarding & Registration Fraud
Ambriel effectively detects fake accounts and synthetic identities during the onboarding process. By identifying these threats early, businesses can prevent exploitation of their platforms and ensure only legitimate users gain access.
Payment & Transaction Fraud
Real-time monitoring of transactions allows Ambriel to spot anomalies and prevent chargebacks. This use case is crucial for maintaining financial integrity and protecting against fraudulent transfers that can harm revenue.
Bonus & Promotion Abuse
By identifying multi-accounting and referral scams, Ambriel helps businesses protect their promotional incentives. This ensures that rewards are distributed fairly and that genuine users are not negatively impacted by fraudulent behavior.
Account Takeover Protection
Ambriel identifies unusual login behavior and device changes, effectively detecting credential stuffing attempts. This proactive approach to account security is essential for keeping customers safe from unauthorized access to their accounts.
Assured
Provider Onboarding
Healthcare organizations can use Assured to onboard new providers rapidly, turning a typically lengthy process into a streamlined operation. With the ability to credential providers in just 48 hours, organizations can significantly reduce the time to revenue generation.
Compliance Management
Assured's real-time monitoring capabilities make it an invaluable tool for compliance management. Organizations can stay ahead of regulatory standards and detect any sanctions well before traditional methods would allow, ensuring ongoing adherence to industry requirements.
Expanding Provider Networks
For organizations looking to expand their provider networks across multiple states, Assured simplifies the licensing and enrollment processes. This capability allows companies to scale efficiently without getting bogged down by administrative complexities.
Operational Efficiency
Healthcare systems can leverage Assured to improve overall operational efficiency. By automating manual tasks, organizations can redirect valuable resources toward patient care and other critical areas, fostering a more patient-centric approach.
Overview
About Ambriel
Ambriel is an advanced fraud intelligence and risk management platform tailored specifically for digital businesses that prioritize security and regulatory compliance. Designed for industries including fintech, marketplaces, retail, and iGaming, Ambriel's primary goal is to protect users while minimizing friction in legitimate activities. By integrating behavioral analytics, device intelligence, and real-time risk scoring, Ambriel creates a comprehensive ecosystem that empowers organizations to proactively detect, score, and prevent various forms of fraud. This capability helps safeguard both revenue and reputation. The platform meticulously analyzes user behaviors, transactions, devices, and network signals to uncover hidden risk patterns and automate mitigation strategies. With its real-time capabilities, Ambriel effectively identifies suspicious activities such as multi-accounting, bonus abuse, referral fraud, synthetic identity creation, payment fraud, and money laundering, ensuring a secure environment for all users.
About Assured
Assured is a cutting-edge, AI-powered provider network management platform designed specifically for healthcare organizations looking to optimize their administrative processes and enhance revenue flow. By automating the complex and often tedious tasks of credentialing, licensing, payer enrollment, and continuous network monitoring, Assured significantly reduces the time and resources typically spent on these activities. It serves provider groups, health systems, payers, and digital health companies, addressing critical challenges such as disconnected data and inefficient manual workflows. The platform's core value proposition lies in its ability to drastically improve speed and accuracy: credentialing takes just 48 hours instead of the traditional 60+ days, with an impressive 95% first-pass approval rate for payer enrollments. Furthermore, Assured enables organizations to detect sanctions 22 days earlier than conventional methods, ensuring compliance and operational efficiency. As an NCQA-certified Credentials Verification Organization (CVO), Assured provides a robust solution that offers real-time monitoring of provider data, all centralized within a single platform, thereby streamlining operations and fostering growth.
Frequently Asked Questions
Ambriel FAQ
What industries can benefit from using Ambriel?
Ambriel is designed for a variety of industries, including fintech, marketplaces, retail, iGaming, insurance, and crypto. Its adaptable features cater to the unique fraud prevention needs of each sector.
How does Ambriel ensure compliance with regulations?
Ambriel automates screening against global sanctions and PEP lists, allowing businesses to maintain compliance without manual checks. This streamlined process helps organizations avoid regulatory pitfalls while focusing on growth.
Can Ambriel integrate with existing systems?
Yes, Ambriel offers integrations with popular platforms like Magento, WooCommerce, and Wix Commerce, making it easy for businesses to incorporate its fraud detection capabilities into their existing systems.
What types of fraud can Ambriel help prevent?
Ambriel effectively prevents a wide range of fraudulent activities, including multi-accounting, bonus abuse, referral fraud, synthetic identity creation, payment fraud, and money laundering, ensuring a secure environment for all users.
Assured FAQ
How does Assured reduce provider onboarding time and administrative costs?
Traditional credentialing processes can take over 60 days due to manual, sequential verifications. Assured streamlines this by processing applications in parallel and integrating with over 2,000 primary sources. Organizations can save approximately $4,200 to $5,800 per provider annually.
What makes Assured more reliable than traditional methods?
Assured's AI-powered platform minimizes human error and delays associated with manual processes. Its automated primary source verifications ensure accuracy and compliance, resulting in a 95% first-pass approval rate for payer enrollments.
Can Assured integrate with existing healthcare systems?
Yes, Assured offers plug-and-play APIs that allow seamless integration with various systems such as ATS, EMR, and Salesforce, enabling organizations to connect their existing technologies effortlessly.
What support does Assured provide?
Assured prides itself on offering the fastest support in the industry, with a response time of under 24 hours. This ensures that organizations receive timely assistance whenever they encounter challenges, maintaining operational continuity.
Alternatives
Ambriel Alternatives
Ambriel is a sophisticated fraud intelligence and risk management platform designed specifically for digital businesses that prioritize security and compliance. It operates within the productivity and management category, offering essential tools to protect revenue and maintain user trust across various transactions. Users often seek alternatives to Ambriel for various reasons, including pricing concerns, the need for specific features tailored to their unique business models, or compatibility with existing platforms. When searching for an alternative, it's crucial to consider factors such as the effectiveness of fraud detection, the breadth of compliance features, and the overall user experience in onboarding and transaction monitoring. In the quest for a suitable alternative, businesses should prioritize platforms that provide robust real-time fraud detection capabilities, comprehensive compliance measures, and seamless integration with their existing systems. Additionally, evaluating customer support, scalability, and user feedback can aid in selecting a solution that aligns with both current needs and future growth. Ultimately, the right alternative should enhance security without adding unnecessary friction to the legitimate user experience.
Assured Alternatives
Assured is an AI-driven provider network management platform designed to streamline the credentialing and enrollment processes for healthcare organizations. By automating these critical tasks, Assured enables providers to begin billing in a matter of days rather than the typical months, making it an essential tool for provider groups, health systems, payers, and digital health companies. Users often seek alternatives to Assured due to factors like pricing, specific feature sets, or compatibility with existing workflows and systems. When considering an alternative, it's vital to assess the platform's efficiency, ease of use, and the extent to which it addresses common pain points in provider credentialing and enrollment. Look for solutions that offer automation, real-time data monitoring, and a proven track record of accuracy and speed.